
Stress less, practice more
Outsourced Medical Billing Services
Get medical reimbursements faster with fewer rejections with our outsourced medical billing services. We provide you with cutting-edge healthcare solutions and improvements to your revenue cycle.
Stress less, practice more
Outsourced Medical Billing Services
Get medical reimbursements faster with fewer rejections with our outsourced medical billing services. We provide you with cutting-edge healthcare solutions and improvements to your revenue cycle.
Specialized medical billing team
Spend more time with your patients
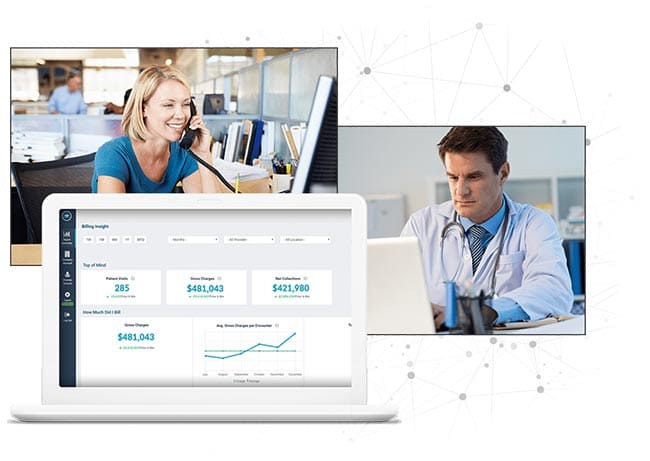
You shouldn’t have to worry about time-consuming and confusing medical billing tasks. Plus, the training and management duties feel insignificant compared to working with your valued patients. Free up your time and mental energy to focus on your patients. Our specialized team is 100% focused on handling your medical billing effectively and efficiently so that you can get paid without the hassle.
Personalized plans & pricing
Built for your practice’s needs
Your practice is unique, so we don’t try to fit it into a box when it comes to our services and pricing. We’ll listen to what your specific needs are and create a personalized plan for you.
Face-to-face Account Managers
We’re here exactly when you need us
Get a US-based, dedicated Account Manager that you can always turn to. Receive regular reports showing how we’re continuing our work for you, plus you’ll always have your personal expert ready to answer any questions that you may have.
Serious savings
An Example Cost Analysis
Inhouse Medical Billing
$1,200,000 in collections
– $100,000 in billing department costs
$1,100,000 in net collections
Outsourced Medical Billing
$1,400,000 in collections
– $100,000 in processing cost & other fees
$1,300,000 in net collections
Coding in all specialties
Work with experts in your specialty
But that’s not all. View all of our specialties.
Testimonials
What our clients are saying
From the blog
Helpful resources
Awards & certifications
Let us be your trusted partner
Magnus Proud Sponsor
Kareo Advisory Board
Kareo Connect Premiere Partner
10 Most Promising Revenue Cycle Management Solution Providers
Magnus Proud Sponsor
Kareo Advisory Board
Kareo Connect Premiere Partner
10 Most Promising Revenue Cycle Management Solution Providers
Is outsourcing right for you?
Calculate how much you can save
Use our free, online calculator to see how much money your practice could save by outsourcing your medical billing. Get your results in 3 easy steps.

Step 1: Call us or submit a form
An expert practice consultant is waiting to serve you
Step 2: Review proposal in one phone call
Analyze your practice’s needs and review services that may increase profitability
Step 3: Finalize your contract
We can start serving you in as little as 5 days
- Step one: Call us or submit a form An expert practice consultant is waiting to serve you
- Step two: Review proposal in one phone call Analyze your practice’s needs and review services that may increase profitability
- Step three: Finalize your contract We can start serving you in as little as 5 days







